B.C. women will now receive an additional crucial insight following a screening mammogram to help reduce their risk of breast cancer.
Starting mid-October, BC Cancer’s breast screening program will now include breast density information with all mammogram results sent to women and their care providers.
The change, announced Friday by Health Minister Adrian Dix, means women will no longer have to request the information themselves. B.C. is the first province in the country to offer this information upfront.
“Breast cancer is the most commonly diagnosed cancer in women in B.C., and we know dense breasts are one of multiple risk factors for this disease,” Dr. Malcolm Moore with BC Cancer said in a statement.
The move follows the completion of an external review by Dr. Andy Coldman, an emeritus scientist in the cancer control research department at the University of British Columbia and the BC Cancer Research Centre. Other recommendations included training for doctors and a communications team to provide other education and support.
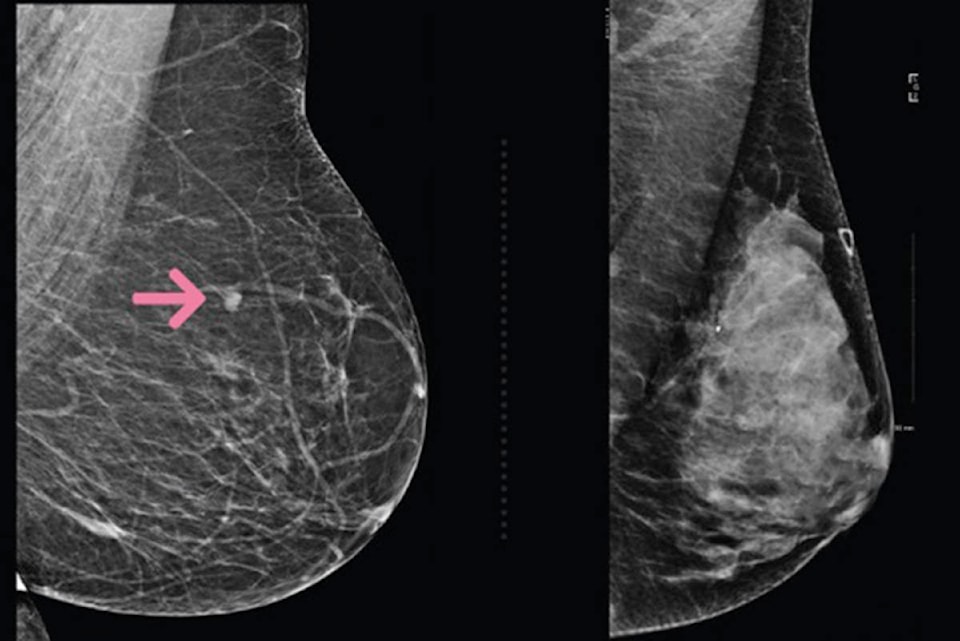
While cancer in a fatty breast is easy to spot, it is often hard for a screening to detect cancer in a dense breast because tissue and cancer both appear white. Roughly 43 per cent of women over the age of 40 have dense breasts, according to Dense Breasts Canada, and considered a greater risk factor than having a family history of breast cancer.
Michelle di Tomaso, co-founder of Dense Breasts Canada, said her group is “thrilled” with the move that will allow women to better understand how their breast density associates with breast cancer risk – an aspect of her health she never had the chance to see.
Her group has been calling for this information to be provided after a screening for years.
Di Tomaso was diagnosed in 2014 with Stage 2B triple positive breast cancer, after being told that her diagnosis had been delayed three years because she had dense breasts.
In the two years after the diagnosis, she underwent two surgeries, chemotherapy, radiation, a double mastectomy and three unsuccessful reconstructive surgeries.
Co-founder Jennie Dale said the information will allow women to decide if they need further screening – something they will either need to pay for privately or try to request through their doctor.
While mammograms catch about 50 per cent of cancers in the densest breasts, ultrasounds can catch an additional three to four cancers per 1,000 women.
“Before [women] were in the dark, they couldn’t talk with their doctor - their doctor didn’t know their breast density, they didn’t know their breast density,” she said.
“Women are still going to need to go get screened privately and advocate very strongly.”
@ashwadhwani
ashley.wadhwani@bpdigital.ca
Like us on Facebook and follow us on Twitter.