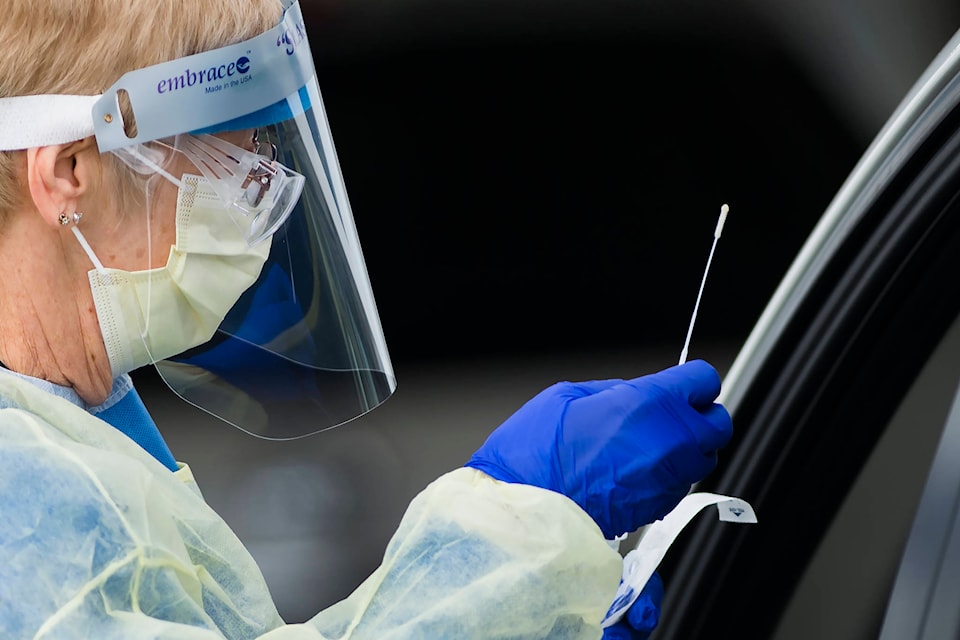
A saliva-based COVID-19 test is likely to be available this fall, say private and public health officials touting various methods under consideration across the country as lineups grow at COVID-19 assessment centres and cases emerge in newly reopened schools.
Public Health Ontario’s chief of microbiology and laboratory science lists several issues to be resolved before broad provincial use but expects saliva collection will soon make it easier to detect infection, especially among children and others unable to tolerate a nasopharyngeal swab.
“I do foresee it being an option in the near term,” Dr. Vanessa Allen said in a recent interview.
“We’re aiming in the space of weeks to months. Sometime later this fall looks very probable.”
While not as accurate as the gold standard method — in which a long, flexible swab is inserted deep into the nostril — saliva collection is easier, meaning this approach could capture infections in people who otherwise would not be tested but should be, says Allen.
To be clear, these are not the at-home saliva tests that generate an immediate result, but lab-based tests that use the same molecular analysis to detect novel coronavirus in a nasopharyngeal sample.
Essentially, the only difference is the type of specimen being collected.
In that regard, the sample is no easier or quicker to analyze because it requires essentially the same trained lab personnel, machinery and chemicals used for traditional methods — some of which were subject to global supply chain issues early in the pandemic.
However, at the collection stage, saliva-based detection could preserve high-demand health resources and supplies, such as personal protective equipment and nurses, says Dr. Jenisa Naidoo, chief scientific officer at the testing and laboratory firm Dynacare.
Naidoo says the company has developed a proven technique that is 98.4 per cent as accurate as the standard nasopharyngeal method.
It allows patients to collect their own specimen, thereby avoiding close contact with a public health nurse who would need PPE.
“So you have preservation of the PPE, you also don’t need the skilled health-care worker to take that sample, which they would do with the nasopharyngeal swab. And you also don’t have a dependency on that swab, that we actually had a shortage of,” says Naidoo, whose study did not test the method on children.
“The patient can literally spit into a vial or tube and you can use that method versus having a swab stuck into their nose or going into their throat.”
It’s also designed to use standard, widely available tubes, which can be found in any laboratory and does not require Health Canada approval, adds a Dynacare spokesman.
The Brampton, Ont.-based Dynacare, which has 231 locations in Manitoba, Ontario and Quebec, says it is developing plans for “the initial rollout with all of our stakeholders in both government and private industry.”
“Given our experience and scale, this will take place first in Ontario,” says spokesman Mark Bernhardt, who adds Dynacare is ramping up capacity by adding staff and equipment.
“The next steps are to optimize our process to permit high-throughput testing using automation. We are hoping to eventually offer saliva collection to the broader public.”
Allen calls Dynacare’s study “quite good.” It tested 432 patients, who provided saliva and nasopharyngeal samples between June 3 and Aug. 1. The nasopharyngeal samples missed four positive cases and the saliva test missed three.
“I think it will be an acceptable method; we need to make sure that we’ve done all the due diligence so that it performs as well as possible,” she says, noting that includes ensuring the main labs can handle saliva.
Canada’s chief public health officer acknowledged Tuesday that multiple places across Canada are investigating the potential of saliva to detect COVID-19 and hinted at efforts to ensure the option is available coast-to-coast.
“We are just trying to look at those results, and standardizing them as well,” said Theresa Tam.
A spokeswoman for British Columbia’s Provincial Health Services Authority acknowledges the province is “looking into alternate collection methods as part of its test planning for the fall” but would provide no details.
One saliva-based approach that seems well-positioned for a national rollout comes from researchers at The Ottawa Hospital and University of Ottawa in conjunction with the National Microbiology Lab in Winnipeg.
It employs a saliva collection kit designed by Kanata, Ont.-based DNA Genotek comprised of a small collection tube with a small funnel at the top. The device is awaiting Health Canada approval for use beyond research purposes.
A study led by cancer surgeon Dr. Stephanie Johnson-Obaseki, who was inspired by her previous work on a spit test for HPV, used the device to collect saliva and nasopharyngeal samples from 1,939 people who visited the Ottawa hospital with either mild or no symptoms of COVID-19.
Johnson-Obaseki says 34 people tested positive with both methods, but 22 tested positive with the swab test alone and 14 tested positive with the spit test alone. The results were published Aug. 28 in Annals of Internal Medicine.
“So each test missed some,” says Johnson-Obaseki, a head and neck cancer surgeon at The Ottawa Hospital, who notes no COVID-19 test is perfect.
She says the findings raise questions about whether different tests may be more suitable at different times of a person’s illness.
“More research will have to be done to drill down when each test is the best to use.”
Meanwhile, Public Health Ontario is focused on logistical issues — Allen says some sites have tried urine containers to collect saliva, but at high volumes this “takes up too much space in a lab.” The microbiologist-in-chief at Toronto’s Mount Sinai Hospital adds they’re simply too big for his lab’s machinery.
Dr. Tony Mazzulli also dismisses containers that come with a stabilizing liquid as too expensive to be worthwhile.
Allen admits there is much to sort out.
“We’re collaborating with colleagues in B.C. to look at how we can get the best container to hold it,” says Allen. ”So it’s very practical, perhaps not-so-exciting stuff.”
Then there’s the amount of saliva required. Allen says initial experiments needed as much as five millilitres — basically a full blood tube container.
“That actually takes quite a while (to fill) so now there’s a lot of work on trying to get smaller volume,” she says.
“It’s a tradeoff — you want the best test and you want to make it as easy as possible.”
For months now, Mazzulli has received saliva samples from patients who find nasopharyngeal swabs — as well as less-invasive nasal and throat swabs — too painful or difficult.
He questions whether saliva collection would alleviate staffing or resource demands, noting patient information must still be documented and patients need direct instruction to do it right.
“If you truly want to do it properly, people are supposed to let the saliva pool in their mouth for several minutes before they spit in the container,” says Mazzulli, adding that if a nurse is present for this step, they would definitely need PPE.
“So now they’re going to be sitting there waiting five or 10 minutes because they’re trying to accumulate saliva so you’re getting true liquid and not just the foamy, dry spit so to speak. That could slow things down rather than speed things up.
Nevertheless, public demand for more testing options is clearly on the rise and with COVID-19 cases rising as flu season approaches, various provincial and public health leaders have voiced their commitment to boosting test capacity.
Allen doesn’t expect saliva-collection to become the new standard, but does believe it can make getting a test faster and easier.
“It would still not be the collection method of choice for very sick individuals — we would still retain the gold standard,” she says.
“But again, it’s thinking of innovative ways to make sure that people can get their tests and that there’s no kind of real or perceived impediment to getting that test.”
Cassandra Szklarski, The Canadian Press
Like us on Facebook and follow us on Twitter.
Want to support local journalism? Make a donation here.