B.C.’s COVID-19 infection rate has continued to turn down since mid-November, with hot spots in the southern Interior, the Northwest and the Fraser Valley, where the highest number of diagnosed cases has been determined since fall.
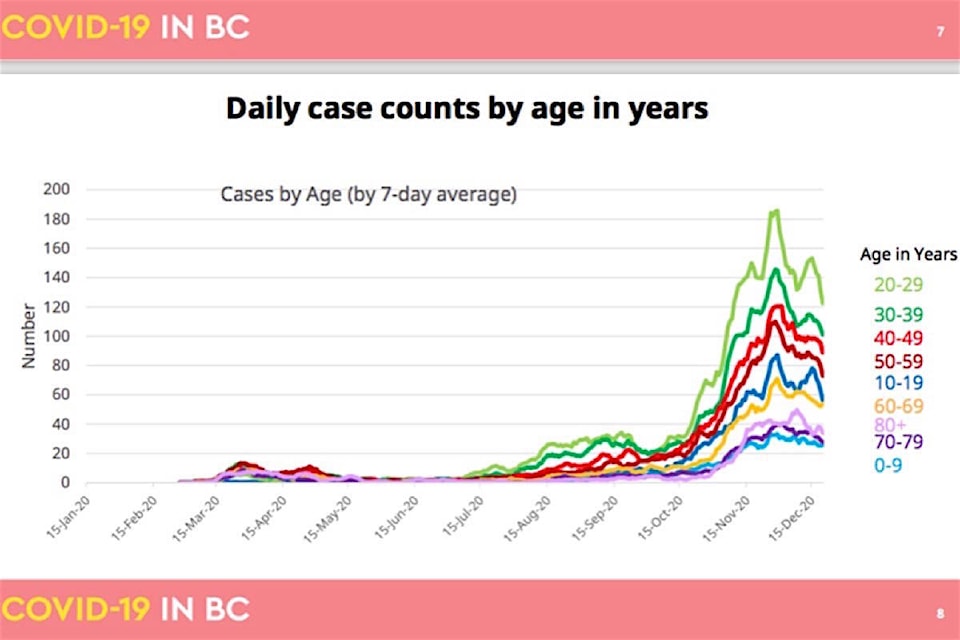
Provincial health officer Dr. Bonnie Henry presented the latest modelling of B.C.’s second surge of coronavirus Dec. 23, showing the age group from 20 to 40 has the highest infection rate. School-aged children continue to test positive at low rates, with fewer than seven out of 1,000 students showing infection as testing ramped up since the start of the school year.
“Most school-aged children who have symptoms do not have COVID-19, and that remains the same as we have seen throughout the pandemic,” Henry said. “With more than 600,000 students and educators back in our school system, this is something that we have been following very carefully.”
She acknowledged that there have been many exposure events, with infected people being in the school environment when they may be contagious.
“We have been posting those regularly,” Henry said. “It does not mean that anybody has transmitted the virus in those settings, but it’s an understanding of how much risk we have in our school environment. And what we have seen is that even though we have exposure events that reflect transmission events in our community, we have very little transmission actually in schools.”
RELATED: 518 new cases Wednesday, death toll nears 800 in B.C.
RELATED: Ottawa approves Moderna vaccine, 40,000 doses on way
Contact tracing to contain community outbreaks has been strained, particularly in the Fraser Health region and in northern B.C., where remote and sparse population is more difficult to reach.
“Most of our cases continue to be linked to a known case or outbreak,” Henry said. “That’s important for us. That means we have not lost the ability to do contact tracing.”
With the second vaccine from Moderna approved for use in Canada, B.C. and other provinces are expecting to start receiving it next week. Pfizer has approved use of its vaccine from more locations outside of the company’s delivery points, allowing more detailed plans, including at-risk remote Indigenous communities.
The first target by the end of February is reaching 150,000 residents and staff of long-term care and assisted living facilities, as well as essential visitors to those facilities, front-line health care workers and 25,000 people in remote and isolated Indigenous communities.
The second priority group for February and March is 400,000 community-based seniors, homeless people, provincial prisons, residential adult mental health patients, long-term care and hospital support staff, community physicians and medical specialists.
@tomfletcherbc
tfletcher@blackpress.ca
Like us on Facebook and follow us on Twitter.