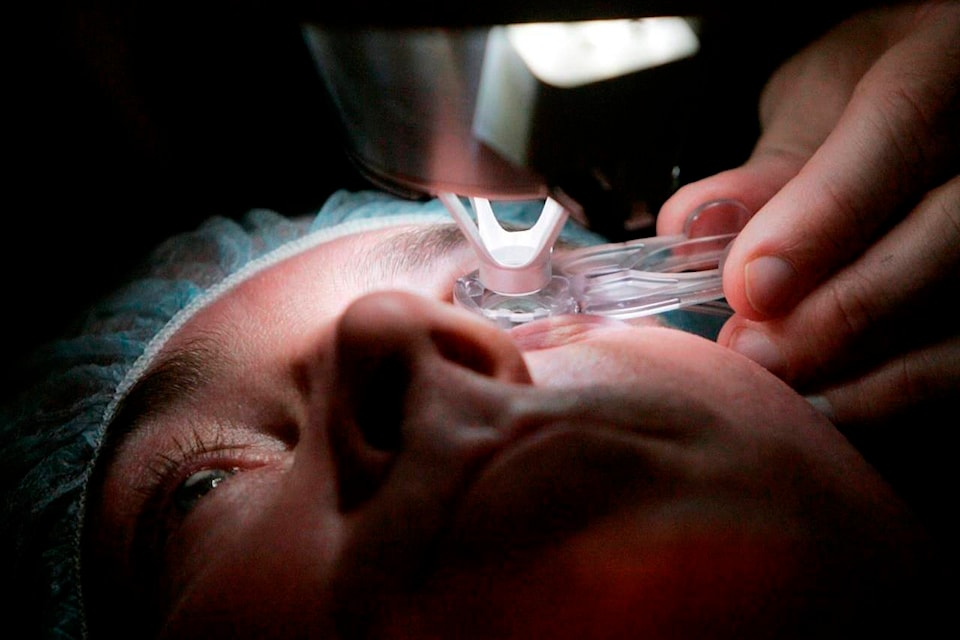
Doctors say they’re becoming increasingly concerned about how they will handle the swelling backlog of elective surgeries once the immediate COVID-19 threat has ebbed.
Hospitals have put off non-urgent surgeries to focus on the viral outbreak.
But doctors worry their elective procedures could become urgent by the time operating rooms are available.
“Our waiting times will increase and it’ll backlog,” said Dr. Sandy Buchman, president of the Canadian Medical Association.
The term elective can be misleading, bringing to mind optional cosmetic surgeries, for example.
But the term really refers to anything that’s not immediately life-threatening, and can include procedures needed to treat serious medical conditions, Buchman said.
Most patients in Canada already wait longer than recommended for their surgeries, according to the Canadian Institute for Health Information.
Only 75 per cent of patients in Canada received hip replacement surgery within the recommended 182 days of when the doctor agreed to the surgery in 2018, for example.
Only 69 per cent of patients needing knee replacements got theirs within the same recommended time frame.
And that doesn’t include the time it takes to get a referral to a specialist.
The number of people who have their surgeries within the benchmark time frames has been slipping slightly but steadily for several years, according to the statistics.
“We have a good system in many ways but our waiting times have always been the bane of our system,” Buchman said.
Buchman knows what life on the waiting list can be like. He received a hip replacement five years ago.
He spent roughly two years waiting for his surgery from the time he first visited his doctor.
“It was bad. I needed surgery and the surgery made a big difference in my life,” he said looking back.
While the need for a hip replacement isn’t life-threatening, waiting an extended period could have a serious effect on a patient’s quality of life, he said, limiting their ability to work.
READ MORE: B.C. hospitals getting some scheduled surgeries done amid pandemic
There are also conditions that might seem relatively benign at first, like gallstones, that can develop into dangerous conditions like sepsis, or blood poisoning, if left too long, he said.
Part of the problem is that surgeons are not going to be able to catch up once hospitals start getting back to those waiting list.
While Buchman hopes the surge in virtual care and telephone appointments may help doctors assess patients more efficiently in the post-COVID-19 world, they won’t be able to suddenly start doing more surgeries than before.
“We aren’t going to bring in more doctors to all of a sudden do twice as many procedures,” he said. “They’re working at 120 per cent as it is.”
Even if surgeons could somehow work safely at greater speed, time in the operating room is limited.
The pandemic has highlighted major gaps in Canada’s systems, and health care is no different.
According to the latest estimate from the Fraser Institute, the total number of procedures people were waiting for across the 10 provinces in 2019 was over more than one million. That meant 2.9 per cent of Canadians waiting for treatment last year.
The results of delays can be devastating, according to Bacchus Barua, the think thank’s associate director of health policy studies.
“Wait times can, and do, have serious consequences such as increased pain, suffering, and mental anguish. In certain instances, they can also result in poorer medical outcomes — transforming potentially reversible illnesses or injuries into chronic, irreversible conditions, or even permanent disabilities,” he wrote in his report late last year.
It’s not clear when hospitals will begin allowing less urgent surgeries to resume, and it will be up to individual provinces to decide.
New federal guidelines say that in order for provinces to begin to reopen their economies, hospitals should have the capacity to handle those procedures, along with any new cases of COVID-19, including access to protective equipment for workers.
Laura Osman, The Canadian Press
Like us on Facebook and follow us on Twitter.