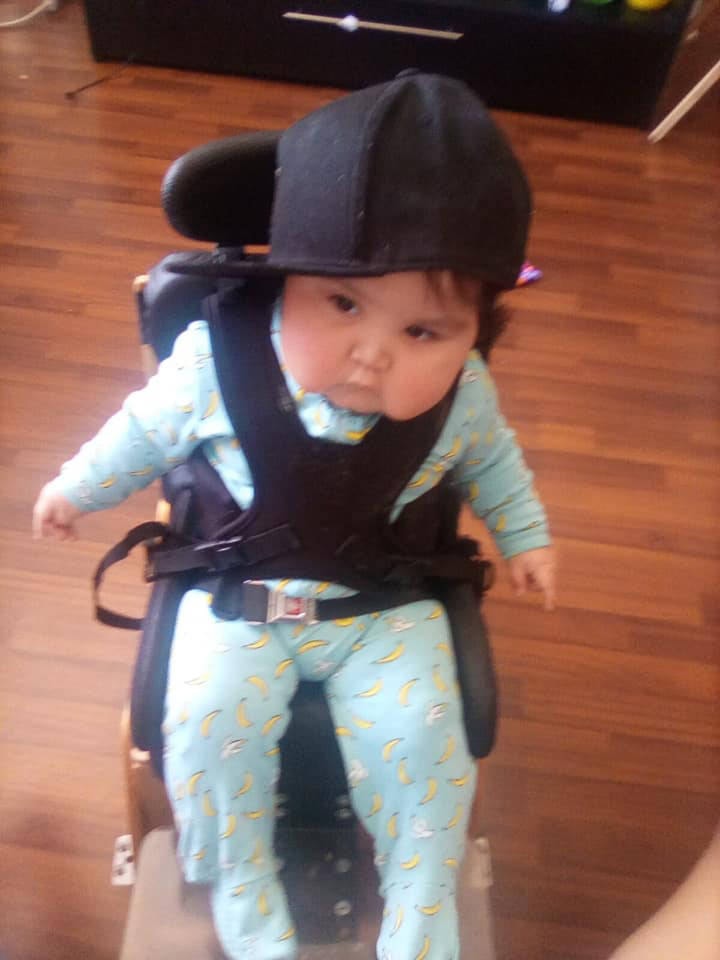
A Nisga’a woman plans to file a lawsuit against Northern Health related to the treatment she received while giving birth to her baby last summer at the University Hospital of Northern British Columbia in Prince George.
Kristy White alleges that due to racism and mismanagement during her delivery, her child Wesley suffered a brain injury.
White said that her baby was in a transverse position and she was 37 weeks pregnant when she arrived in Prince George to deliver the baby on June 17, 2020.
She alleges that a nurse made racially insensitive comments, and kept her and Wesley’s father Warren alone for nearly her entire shift on June 18.
White said that the nurse’s comments started when she was trying to have a conversation with her about traditional Indigenous foods.
“When we were trying to explain it to her, she’s like, ‘I don’t understand why you people do those kinds of things,’ and she wrinkled her nose, threw her hands in the air,” White said.
She would often say ‘Indians’ like she’s being biased towards me.”
White alleges that the nurse did not include her in any decisions about her care, and when a doctor instructed the nurse to increase the dose of oxytocin, the nurse initially refused to do so, resulting in White being unable to become fully dilated.
“You know how somebody who’s caring and compassionate and trying to help you get through something like a nurse normally would, she wasn’t that way, she was very biased,” White said.
“She was very rude, very ignorant. It was hard to have any conversations with her, she wouldn’t let me speak for myself.”
Doctors attempted a vacuum-assisted delivery, which White claims to have caused the infant to suffer injuries. On May 3, 2021, a neurologist at the BC Children’s Hospital in Vancouver diagnosed Wesley with brain bleeds, and White said the neurologist told her the damage was likely due to the vacuum-assisted birth.
According to White, Wesley is behind his physical development by around six months and requires physiotherapy, occupational therapy and speech therapy as well as trips to the BC Children’s Hospital every three months.
After the birth, the Whites submitted a complaint to Northern Health’s Patient Care Quality Office. Northern Health determined that racism did not play a role in the nurse’s actions.
But the agency did acknowledge in an August 2020 email sent to Kristy White that there was a disagreement between the nurse and doctor, resulting in the medical team not functioning effectively and that management was working with the nurse to “ensure she understands the impact of her actions and that she will become a more effective team player in the future.”
White has also submitted a complaint to the College of BC Nursing Professionals and is now working with Pacific Medical Law, a Vancouver-based firm specializing in medical malpractice and birth injury. She said she plans to file a lawsuit in the coming months after obtaining all of Wesley’s medical records.
“I’ve kept quiet because I’m not the type of person to be public about my life and what I’m going through – my focus is Wesley, it’s always going to be Wesley.”
“I don’t want this to happen to anybody else. I’m speaking out because there needs to be a change.”
Northern Health said in a statement that it cannot comment on specific patient experiences to protect their privacy, but that there was a quality of care complaint investigated when concerns were raised in June 2020 and the results were provided to the complainant.
“Anyone who is unsatisfied with the response or outcome from a health authority Patient Care Quality Office investigation, also has the option of contacting the Patient Care Quality Review Board for an independent review,” the statement reads.
“Northern Health strives to support a health care system that is culturally safe for Indigenous people; we are committed to providing a work and care environment that is characterized by respectful behaviour, and free from discrimination, bullying and harassment. We know that the vast majority of our staff and care providers share this commitment, and provide culturally safe care every day – and we also know there is more work to be done.”
READ MORE: Kitimat hospital care review result won’t be made public