Taking illicit drugs is like playing Russian Roulette, says an Interior health official.
Unlike Vancouver, where television reports on the opioid crisis almost daily, the B.C. Interior does not get much play. But opioids are very much a problem in this region as well.
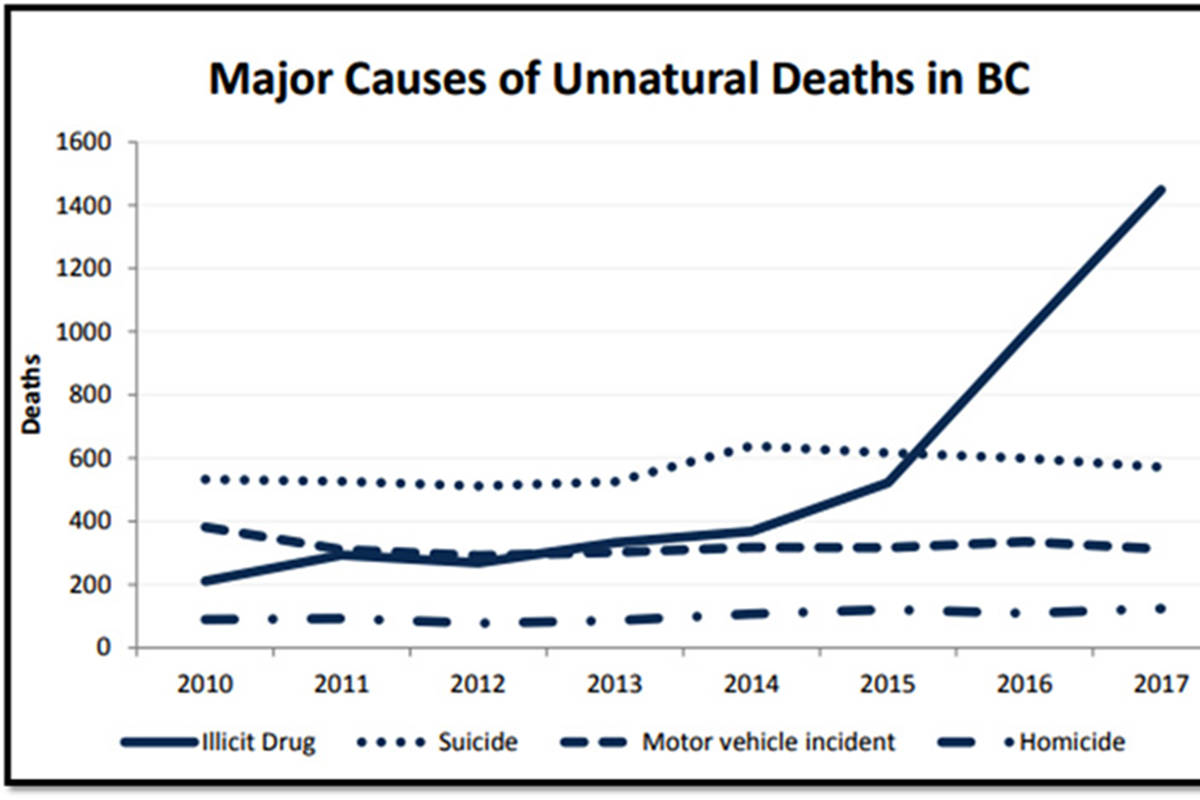
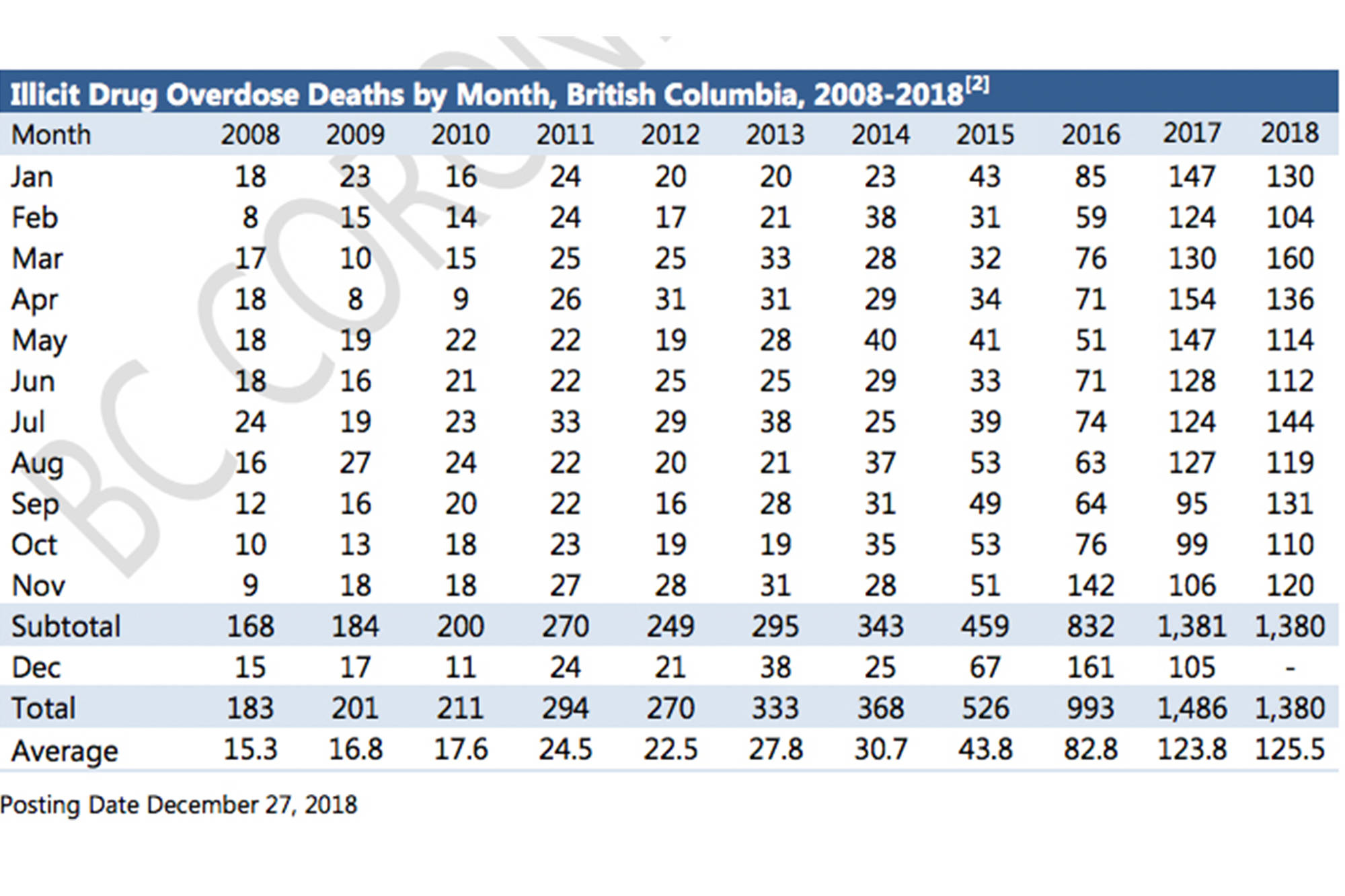
A BC Coroner’s Report that provides confirmed and suspected illicit overdose deaths, indicates that between Jan. 1 and Nov. 30, 2018, Vancouver Coastal Health Authority had the highest rate of illicit drug overdose deaths (37 deaths per 100,000 individuals) followed by Interior Health Authority (31 deaths per 100,000 individuals) for the same period.
In Interior Health, the rates were highest in Thompson Cariboo and Okanagan health service delivery areas.
Related: B.C. doctors told not to limit opioids or refuse care of chronic pain patients
“Overdose deaths, followed by loss for family and friends is a result of the Russian Roulette users of illicit drugs engage in,” says Megan DeSimone, IHA Mental Health and Substance Use North Okanagan community manager.
She says that in the past, illicit drug users were fairly confident they were getting what they ordered when they made their illicit drug purchases.
No longer.
“The drugs are now high-risk; there’s poison in the drugs and we’re not just talking about heroin,” she says, reminding that illicit drug makers do not create their drugs in meticulously clean labs, and even marijuana sold on the street can be contaminated with fentanyl. “By the very nature of fentanyl, if it’s in the building, heroin, cocaine, any of the drugs you would think of, including Ecstasy, it could be in there too.”
Retired Salmon Arm nurse Wendy Piccini is well aware of the local crisis. Two of her sons have lost dear friends to overdoses.
“Our oldest son’s best friend died from an overdose in Revelstoke and our second-oldest son went to the funeral of a very good friend in Salmon Arm about two months ago,” she says, noting she and her husband know of several other deaths due to overdose in the Shuswap although not all have been revealed as such. “I think sometimes the families don’t want to say it’s an overdose.”
Related: Moms of those killed by illicit opioids take to B.C. Legislature in call for action
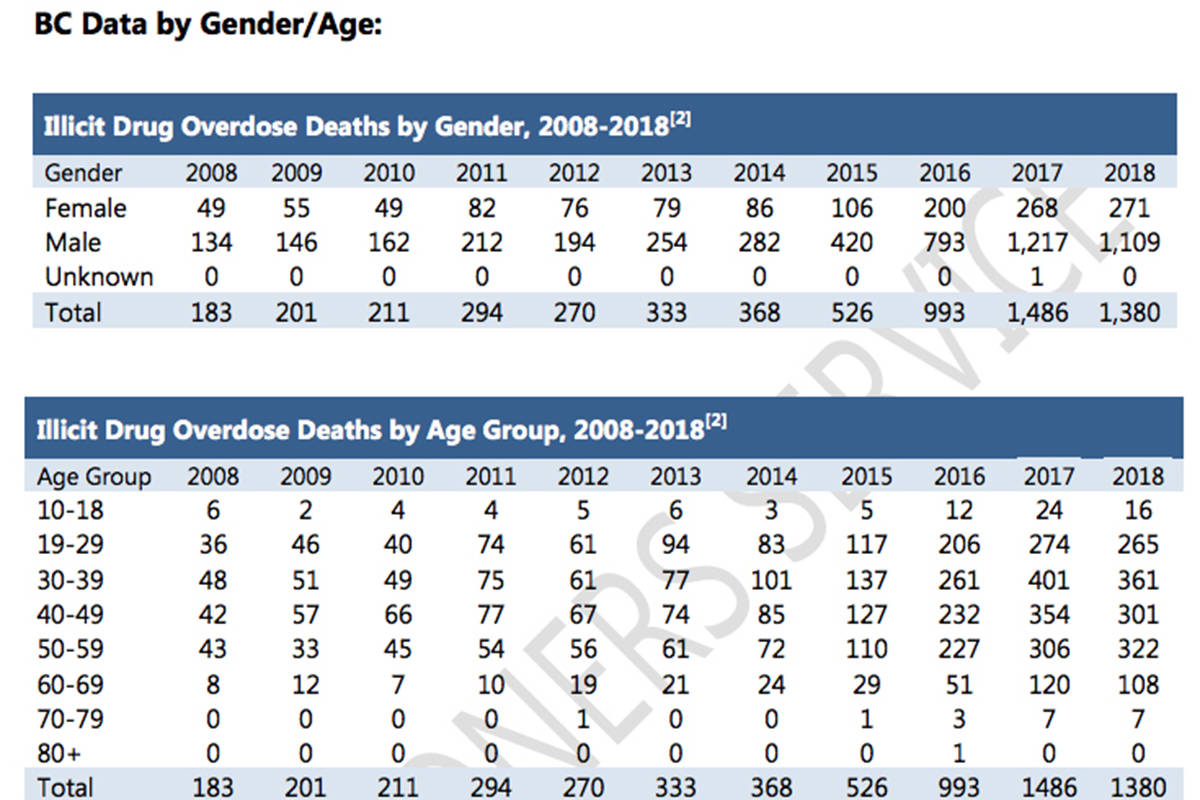
Piccini says most of the deaths she and her family are aware of were individuals between the ages of 30 and 40.
“The one in Revelstoke had a child; they’re in that age group where they often have a wife, or a girlfriend or a live-in, and they’re in the prime work age,” she says, noting she has recently heard that the opioid crisis is now affecting youths between the ages of 10 and 20. “It’s heartbreaking for our two older sons who have lost two best friends and one very good friend.”
DeSimone concurs, noting substance use crosses “all socio-economic barriers, every facet of life, the whole spectrum.”
But help is available.
“If people are ready for treatment and harm-reduction approaches, services are always better in larger centres, but Salmon Arm does have options,” she adds.
Opioid Agonist Treatment or OAT, is the first line of treatment, with entry into the program available by going to the second floor of the Canadian Mental Health office in Salmon Arm on Mondays, Wednesdays and Fridays from 1 to 3 p.m.
“OAT is a long-term treatment that helps control cravings and withdrawals from opioids,” says DeSimone, noting specialized substance-use clinicians are available. “When people are in the throes of opioid addiction, it’s almost impossible to move to the next stage – all people can think of is their next fix. “We need to keep them alive long enough to get them out of that.”
Once they’re stabilized and with the help of a therapist, DeSimone says people can start on a recovery plan to improve their quality of life.
Related: Tailored response in Alberta, B.C. for South Asians addicted to opioids
She explains the OAT therapy is safe and cautions people against going through withdrawal without the therapy.
“Tolerance to opioids reduces substantially, even as much as a couple of days without it,” she says. “If you go back to using (fentanyl) at the same level, there’s a very high risk of overdosing.”
There is evidence, she says, that people who have been on OAT therapy for a year have a “substantial likelihood” of remaining opioid free.
Between 150 and 175 people have accessed the OAT program in the Salmon Arm office where Naloxone kits and training are also available and encouraged.
“The training only takes a couple of minutes; my 14-year-old knows how to do this and carries a kit in a knapsack,” DeSimone says, pointing out people should not feel embarrassed to seek help for opioid addiction. “The least judgmental people you will ever come across are substance-use clinicians. They start where the person’s at, they walk with you and are part of your recovery.”
@SalmonArm
barb.brouwer@saobserver.net
Like us on Facebook and follow us on Twitter